
Let’s face it: navigating the world of medical insurance feels like trying to solve a puzzle in the dark. You’ve found the perfect electric wheelchair—one that could give you back your independence—but the price tag looks like a down payment on a car. With costs ranging from
1,200toover1,200 to over 1,200toover
30,000, the first question everyone asks is, “Am I going to have to pay for this myself?”
The short answer is yes, usually—but only if you can successfully navigate the complex “fiscal fortifications” erected by providers like Medicare and private insurers.
Here is the gist if you are in a hurry:Most insurance plans, including Medicare Part B, Medicaid, and private insurers, cover electric wheelchairs, but coverage is strictly conditional based on “medical necessity.” This means you must prove you need the device for daily activities (like dressing or eating) inside your home, not just for outdoor convenience. Medicare Part B typically covers 80% of the approved cost, leaving you with a 20% coinsurance, while Medicaid and the VA may offer full coverage depending on your eligibility.
In this guide, I’ll walk you through the exact eligibility checklists, the hidden “home use” traps, and a 6-step roadmap to get your claim approved so you can regain your freedom without emptying your savings.
1. Introduction: Mobility, Freedom, and the Financial Reality
The Growing Need for Power Mobility
We are living in an era where mobility is more than just movement; it’s independence. With an aging global population and disability rates on the rise, the demand for power mobility is exploding. The market is projected to reach a staggering $9.05 billion by 2030, driven by innovations in everything from compact travel scooters to the comprehensive wheelchair series available today.
But for the average person facing a mobility challenge, those market stats don’t matter as much as one simple, terrifying question: How am I going to pay for this?
The Insurance Landscape
Navigating this system falls into four primary buckets in the United States:
- Medicare: The biggest player for seniors (65+) and those with specific disabilities.
- Medicaid: State-based aid for low-income individuals.
- Private Insurance: Employer or individual plans (Blue Cross, Aetna, etc.).
- The VA: Specialized, often more comprehensive benefits for veterans.
What We Will Cover
This isn’t just a list of rules. This is your battle plan. We are going to walk through exactly how to navigate eligibility, how to minimize those scary out-of-pocket costs, and how to fight back if you get a denial letter. We will cover specific terms like power mobility devices and the prior authorization process so you can speak the language of the insurers and get the equipment you deserve.
2. The “Golden Rule” of Coverage: Understanding Medical Necessity
If you take only one thing away from this article, let it be this: Insurance companies do not care about your comfort; they care about your function.
To get approved, you generally must prove that the device is needed to perform Mobility-Related Activities of Daily Living (MRADLs). These are the non-negotiable basics of survival:
- Toileting
- Feeding
- Dressing
- Grooming
- Bathing
The “Least Costly Alternative” Principle
Insurers operate like accountants. They look for the “Least Costly Alternative.” If a
50canesolvestheproblem,theywon′tbuya50 cane solves the problem, they won’t buy a 50canesolvestheproblem,theywon′tbuya
5,000 scooter. If a manual wheelchair works, they won’t approve a power chair.
This is where documentation becomes critical. Your doctor cannot just say you “need” a power chair. They have to explicitly document why a manual chair fails you.
- Do you lack the upper body strength to self-propel?
- Do you have a respiratory condition that makes manual exertion dangerous?
- Do you require specific spinal alignment features?
For example, if you require specific seating to prevent pressure sores or manage complex spinal issues, documenting the need for an ergonomic electric wheelchair becomes essential. If the paperwork doesn’t explain why the standard seat causes you medical harm, the claim for the ergonomic model dies.
The “Home Use” Restriction (The Medicare Trap)
This is the rule that catches most people off guard. Especially for Medicare Part B coverage, the medical necessity is determined by your need to use the chair inside your home.
If you can walk around your kitchen but need a scooter to go to the grocery store, Medicare will typically deny the claim. They view community mobility as a “convenience,” not a medical necessity. To get coverage, the chair must be required to get you from your bedroom to your bathroom or kitchen.
3. Medicare Part B: The 80/20 Rule and Eligibility
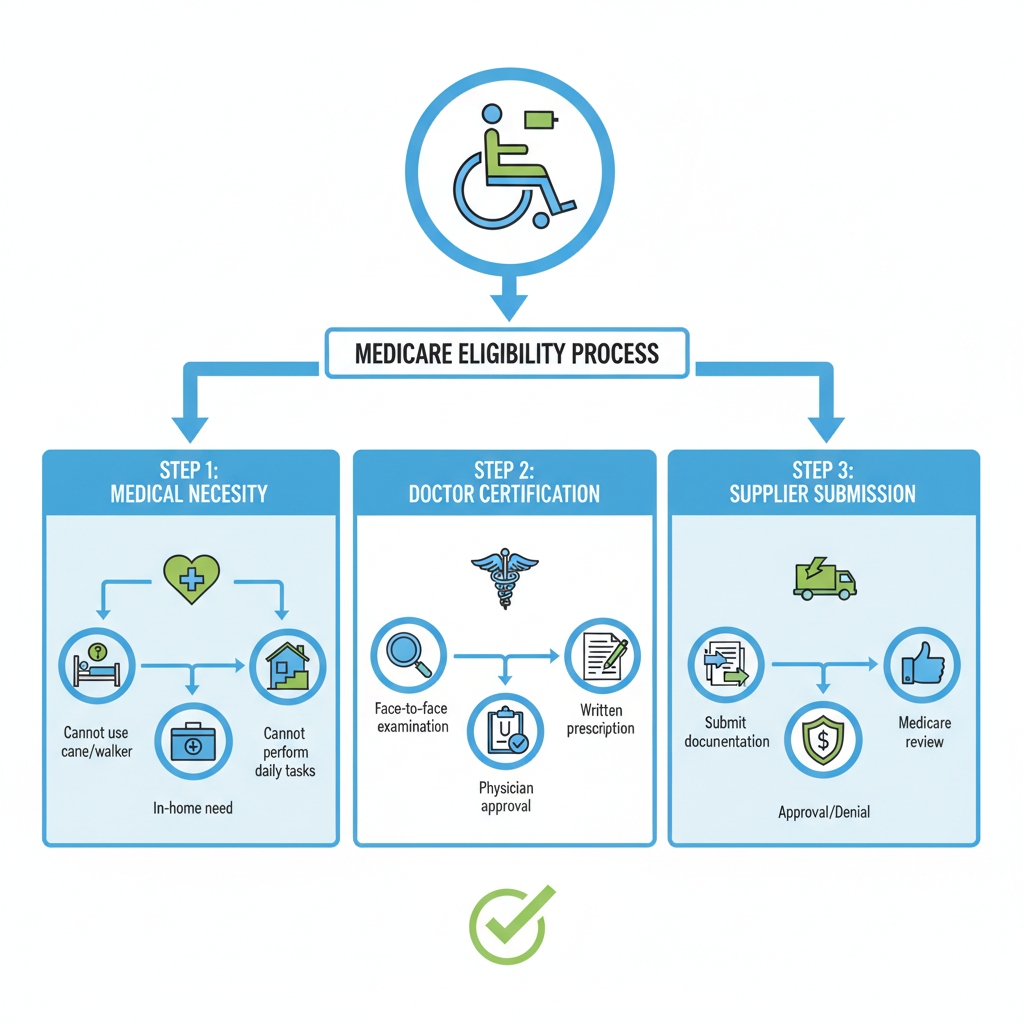
The Durable Medical Equipment (DME) Classification
Medicare classifies electric wheelchairs and scooters as Durable Medical Equipment (DME). This category is for items that withstand repeated use, are primarily for a medical purpose, and are generally not useful to someone who isn’t sick or injured.
Financial Breakdown (2025 Update)
Let’s talk money. Even if you get approved, “covered” rarely means “free.”
- The Deductible: First, you must meet your annual Part B deductible, which is $257 in 2025. You pay this before Medicare pays a dime.
- The 80/20 Coinsurance Rule: Once the deductible is met, Medicare pays 80% of the “Medicare-approved amount.” You are responsible for the remaining 20%. On a 10,000complexrehabchair,thatisa10,000 complex rehab chair, that is a 10,000complexrehabchair,thatisa2,000 bill landing in your mailbox.
The 5-Year Rule
Medicare operates on a 5-year replacement rule. Generally, they will only pay for one mobility device every five years. If your chair breaks in year three and it’s cheaper to replace than repair, they might cover it. But if you just want a newer model? You’re paying cash.
Exception: If your medical condition changes drastically (e.g., a progressive disease requires different seating support), you can sometimes override this rule with strong documentation.
Medicare Advantage (Part C)
If you have Medicare Advantage (Part C), you are dealing with a private company (like Humana or UnitedHealthcare) that manages your Medicare benefits. By law, they must offer at least the same coverage as Original Medicare. However, their copays might be flat fees rather than percentages, and their networks are stricter. Always check your specific plan’s “Evidence of Coverage.”
4. Medicaid: State-Based Coverage and 100% Funding Potential
While Medicare is federal, Medicaid is state-run. This means your location determines your destiny.
The “Medically Needy” Standard
Medicaid eligibility requirements are generally tied to income and resources. However, many states have a “Medically Needy” program (often called a “spend-down” program) that allows individuals with higher incomes to qualify if their medical expenses—like a $15,000 wheelchair—eat up their disposable income.
Coverage Differences by State
- The Good News: In many states, if you qualify, Medicaid covers 100% of the cost of Durable Medical Equipment (DME). No deductibles, no 20% coinsurance.
- The Bad News: States often have much stricter “approved lists” (formularies) of equipment. You might get a standard chair but be denied specific upgrades unless strictly medically proven.
Dual Eligibility: The Sweet Spot
If you are “Dual Eligible” (qualifying for both Medicare and Medicaid), you are in the best financial position. Medicare pays the first 80%, and Medicaid typically picks up the remaining 20% coinsurance, theoretically reducing your out-of-pocket costs to zero.
Institutional Coverage Updates
Historically, people in nursing homes faced hurdles getting customized chairs. However, legislative updates are changing this. For example, New Jersey Bill S3438 recently reinforced the rights of nursing facility residents to access specialized motorized wheelchairs, ensuring that institutionalization doesn’t mean a loss of mobility rights.
5. Private Health Insurance: Navigating Employer and Individual Plans
Private health insurance plans are the Wild West. One PPO plan might cover 90% of a chair, while an HMO plan might only cover 50% and restrict you to a single supplier. You must read your “Summary of Benefits” specifically looking for the “Durable Medical Equipment” section.
The Prior Authorization Hurdle
Unlike Medicare, which sometimes allows suppliers to ship and bill later (though this is changing), private insurance almost always demands a prior authorization process. This means the insurer must sign off on the specific make, model, and price before the order is placed.
Network Restrictions
You must use an “In-Network” DME provider. If you buy a chair from an online retailer that isn’t in your network, your insurance may pay nothing, treating it as an out-of-network elective purchase.
Replacement and Repairs
Private policies can be tricky regarding repairs. While government plans are standardized, private insurers often have caps on labor costs for repairs. Always ask: “Does this policy cover battery replacements?” Batteries for power chairs are expensive and wear out every 1-2 years.
6. Veterans Affairs (VA) Benefits: Comprehensive Support for Heroes
VA disability benefits are arguably the best coverage available, but they prioritize effectively.
- Service-Connected: If your disability is a result of your service, the VA typically covers 100% of the cost of the wheelchair and any necessary accessories.
- Non-Service Connected: Veterans with non-service-connected disabilities can still qualify, but it is based on financial need and medical necessity.
Full Coverage Potential
The VA differentiates itself by looking at the “whole person.” Unlike Medicare’s “in-home” restriction, the VA often considers your need to leave the house for appointments and social integration. They frequently cover full costs, including ramps and lifts for your vehicle or home.
Specific Conditions
Certain conditions trigger automatic eligibility for specific benefits. Veterans with ALS, loss of use of limbs, or severe vision impairment (20/200 or less) often see a streamlined approval process.
7. The 6-Step Roadmap to Approval: From Doctor to Delivery
Getting a power chair isn’t like buying a car; it’s a medical prescription process. Follow these steps to avoid the dreaded denial.
- The Face-to-Face Mobility ExaminationYou cannot just call a supplier. You must have an in-person (or approved telehealth) exam with your treating physician. The doctor must document that you have a mobility deficit that impairs your daily life and that a manual chair is insufficient.
- Pro Tip: Ensure the notes say: “Patient cannot self-propel a manual wheelchair due to [specific condition].”
- The “7-Element Order”Your doctor must generate a specific power wheelchair prescription. It must include: Beneficiary’s name, Description of the ordered item, Date of exam, Diagnoses, Length of need, Physician’s signature, and Date of signature.
- The Letter of Medical Necessity (LMN)This is the most important document in the stack. A generic note won’t cut it. The LMN must be a narrative explaining your day-to-day life. It connects the dots between “Patient has MS” and “Patient cannot feed themselves without a power chair featuring seat elevation.”
- The Home AssessmentBefore Medicare pays, they often require a home assessment. A supplier will visit your home to verify doorways are wide enough and flooring is suitable. If your home can’t accommodate the chair, they won’t pay for it.
- Supplier SelectionYou must choose a Medicare-enrolled supplier (or in-network provider). Crucially, ask if they “accept assignment.” If they do, they agree to accept the Medicare-approved amount as payment in full. If they don’t, they can charge you excess fees that insurance won’t touch.
- Delivery and TrainingUpon delivery, the supplier isn’t just dropping off a box. They are required to train you. You must demonstrate that you can safely operate the equipment. If you can’t drive it safely, they can’t leave it.
8. Out-of-Pocket Costs: What You Should Expect to Pay
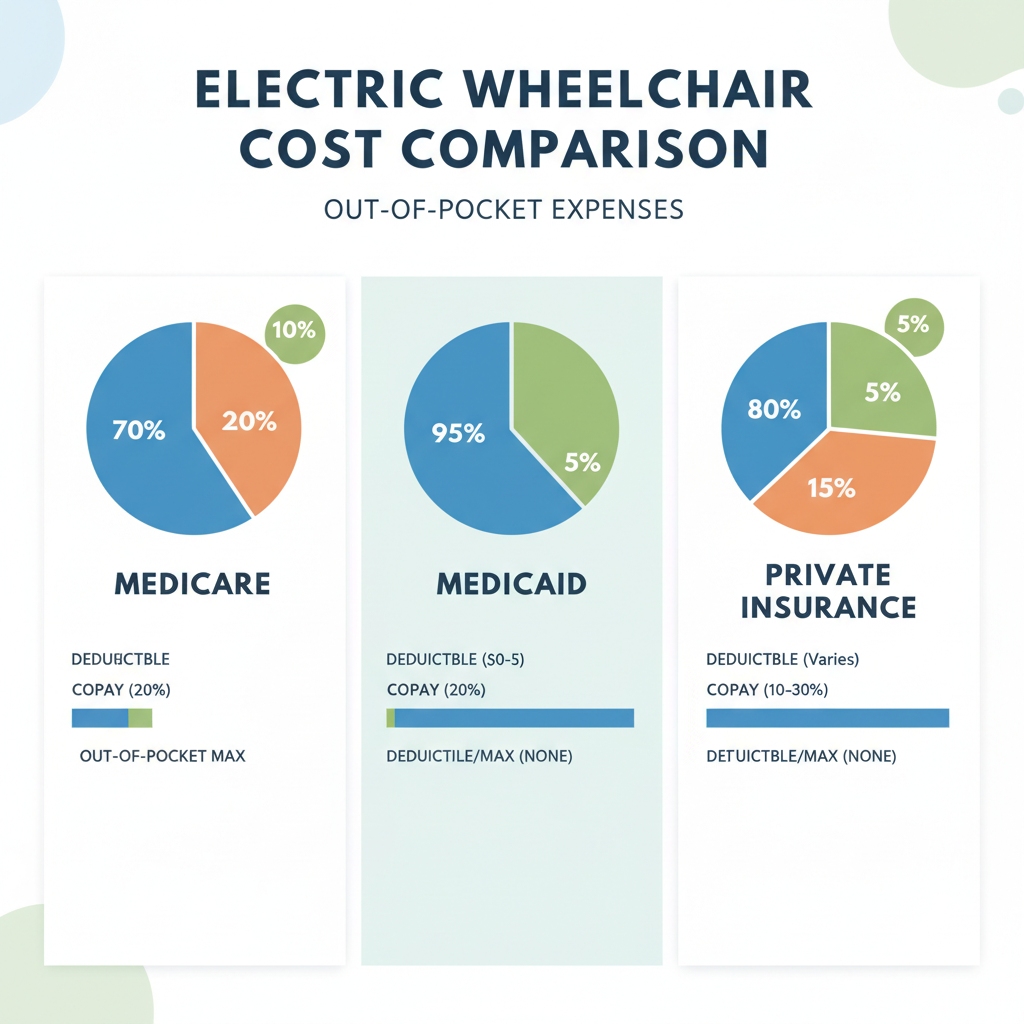
Deductibles and Co-Pays
Let’s be realistic. If you are on Medicare Part B, and you haven’t met your deductible, you are paying the first **
257∗∗.Then,forastandard257**. Then, for a standard 257∗∗.Then,forastandard
6,000 power chair, your 20% coinsurance is $1,200. That is a significant chunk of change for many seniors.
Upgrades and “Luxury” Features
Do you want a specific color? Rugged tires? High-speed motors? Insurance views these as “not medically necessary.”
This scrutiny extends to sizing. For example, while standard sizes are routine, wide-seat electric wheelchair models required for bariatric patients are covered, but they require specific Body Mass Index (BMI) documentation to prove that a standard seat would be unsafe or cause injury. If you want the upgraded model purely for comfort rather than medical necessity, you will likely pay the difference via an Advance Beneficiary Notice (ABN).
Alternative Funding
If the out-of-pocket costs are too high, look into:
- Health Savings Accounts (HSA) / Flexible Spending Accounts (FSA): Pre-tax dollars can be used for the copay.
- Non-profits: The ALS Association or MS Society often have loaner closets or grant programs.
- Supplier Financing: Many large suppliers offer payment plans.
9. Recent Policy Updates (2024-2025): Changing the Game

Seat Elevation Victory
For years, Medicare denied “seat elevators” (mechanisms that raise the user to eye level) as “convenience items.” However, a massive advocacy win in May 2023 changed this. CMS now recognizes seat elevation system coverage as medically necessary for certain power wheelchairs. This allows users to reach countertops and transfer surfaces safely.
Telehealth Flexibility
Post-pandemic regulations have shifted. In many cases, the mandatory face-to-face mobility examination can now be conducted via telehealth, provided it includes a video component where the doctor can visually assess your mobility limitations.
Advanced Technology Recognition
Insurers are slowly warming up to complex rehab technology (CRT). This involves individually configured systems with advanced electronics. However, not all tech is treated equally. While standard power mobility is covered, highly advanced terrain features like a stair-climbing wheelchair are still frequently categorized as luxury items or “not medically necessary” for in-home use. If you require this level of technology for environmental access, be prepared for a rigorous appeals process or alternative funding sources.
10. Denials and Appeals: Don’t Take “No” for an Answer
Receiving a denial letter is heartbreaking, but it’s common. The usual suspects include:
- “Not Medically Necessary”: The insurer thinks you can use a cane or manual chair.
- Clerical Errors: The doctor forgot a date, or the signature is illegible.
- Failure to Rule Out Lower Options: The notes didn’t explicitly state why a scooter (POV) wouldn’t work, so they denied the power chair.
The Appeals Hierarchy
You have rights. Use them.
- Internal Appeal: This is asking the insurer to check their math. Often, submitting a corrected LMN fixes this.
- External Review: An independent third party reviews the case.
- ALJ (Administrative Law Judge): If you are on Medicare, this is your ace in the hole. Statistics show that up to 96% of denials are overturned at the ALJ level. It takes time, but the odds are in your favor.
11. Essential Tips for Ensuring Approval
- PT/OT Involvement: Do not rely solely on your General Practitioner. Get a Physical or Occupational Therapist involved early. They speak “insurance language” fluently and their evaluations carry massive weight.
- Drafting the Narrative: Encourage your medical team to use specific phrasing. Instead of “Patient has trouble walking,” use “Patient is bedbound without this device and cannot perform toileting activities independently.”
- Track Everything: Keep a binder. Every prescription, every denial letter, every phone call timestamp. If a supplier loses your paperwork (which happens), you need copies.
12. Conclusion: Reclaiming Mobility
Getting an electric wheelchair covered by insurance is a journey through bureaucracy, but it is a journey you can win. Remember the trifecta: Medical Necessity, Proper Documentation, and Persistence.
Whether you are dealing with the 80/20 coinsurance rule of Medicare or the strict networks of private plans, the key is proving that this device is the only thing standing between you and your basic daily independence.
Don’t let the paperwork scare you. The funding is there. If you are confused by your specific policy, contact a local SHIP (State Health Insurance Assistance Program) counselor—they provide free, unbiased guidance to help you navigate these exact waters.
Reclaim your freedom; you’ve earned it.
